Total shoulder replacement, also known as total shoulder arthroplasty (TSA), is a tremendously successful procedure for treating the severe pain and stiffness that often result at the end stage of various forms of arthritis or degenerative joint disease of the shoulder joint.
The primary goal of shoulder replacement surgery is pain relief, with a secondary benefit of restoring motion, strength, and function.
Doctors recommend joint replacement surgery when shoulder pain and loss of function become severe and when medicines and other treatments no longer relieve pain.
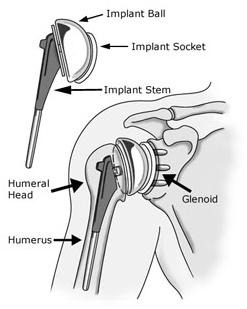
The surgery involves replacing the humeral head (or joint “ball”) and the glenoid (called the “socket”).
Anatomy of the shoulder area, depicting the implant
after surgery. Partial shoulder replacement (or hemi-replacement) may also be indicated with certain severe shoulder fractures of the humeral head. This technique requires the replacement of that component only.




Cancer Treatment in India, VSD Closure (Ventricular Septal Defect), ASD Closure Surgery (Atrial Septal Defect), Heart hole closure surgery in india, Brain Tumour Surgery in India, Craniotomy Surgery for Treatment of Brain Tumour in India, Brain Stem Glioma Treatment in India, Deep Brain Stimulation surgery in india , Best Spine Surgery In India , Cervical Spine Disorders Surgery and Treatment in india , epilepsy surgery in india , Heart Surgery in india , Best open heart surgery hospital in India , All about Spine Surgery, Types of Back Surgery , Top Doctors In India , Best Hospitals in India , Bhavin Desai cardiac surgeon, Best kidney transplant doctor in IndiaBest hospital for limb lengthening surgery in India, Best hospital for neurosurgery in India, Best hospital for bypass surgery in India, Narayana Hrudayalaya online appointment, Best orthopedic hospital in Bangalore, Best open heart surgery hospital in India, Best bypass surgeon in India, best spine surgery hospital in India, Artemis hospital Gurgaon, KD hospital medical appointment
Limb lengthening surgery cost in India, DSA test, Diabetes treatment in India